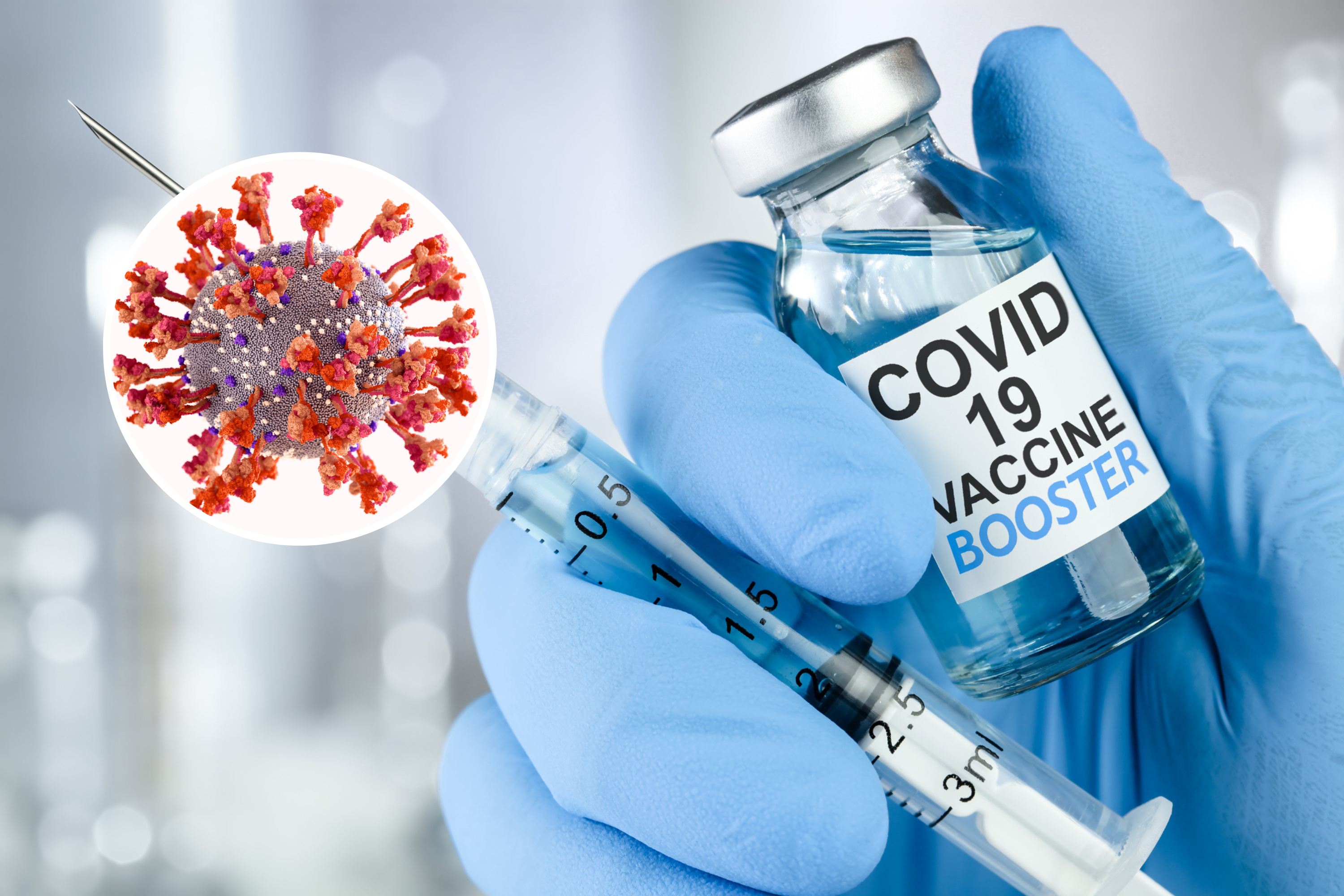
Scientists have warned of a “summer wave” of COVID-19 infections after a highly transmissible new group of omicron subvariants was detected in the U.S. But will our vaccines stand up to these new strains?
Nicknamed FLiRT, the new class of COVID subvariants has quickly spread through the U.S., with one strain, KP.2, becoming the dominant strain of coronavirus in the U.S. as of May 11, according to the U.S. Centers for Disease Control and Prevention.
Read more: Compare Top Health Savings Accounts
Their nickname, FLiRT, derives from the position of the mutations in their spike proteins—projections on the virus surface that allow them to enter our cells. These proteins are also used as a target by our immune system and vaccinations.
So what do these mutations mean for our immunity against the new strains?

SilverV/Getty
“The FLiRT subvariants are direct descendants of JN.1, the previous subvariant that has dominated the world since late last year,” Adrian Esterman, an epidemiologist and professor of biostatistics at the University of South Australia, told Newsweek. “The FLiRT subvariants are more infectious than JN.1 due to a small number of mutations in the spike protein that better help the virus evade our immune system.”
However, despite these differences, Esterman said, the current vaccines would still provide some level of immunity against these variants.
“Even though the FLiRT subvariants are now quite genetically distant from the XBB subvariants—the current vaccine is based on XBB.1.5—the vaccine will still give some cross-immunity against them,” he said. “[However,] there will be a new vaccine available around September, based on either JN.1 or one of the FLiRT subvariants, that will give much better protection.”
Newsweek previously spoke to Lawrence Young, a professor of virology and molecular oncology at the U.K.’s University of Warwick. He agreed that while the currently available vaccines might not be a “perfect match,” they are still likely to provide some level of protection.
So should we be concerned about FLiRT?
“These are early days yet, with the new FLiRT subvariants only being reported in the last week or two,” Esterman said. “So current understanding of these subvariants’ severity may change. [However,] it looks very much like we will see a similar pattern to when JN.1 hit. Because of increased transmission, I do expect case numbers, COVID-19 hospitalizations and COVID-19-related deaths to increase, but nowhere near as high as earlier in 2023.”
From what we know so far, he added, most infected adults experience the new variants as a typical flu-like illness which they will get over in a couple of days. “Probably, the biggest concern is the potential for long COVID, especially after repeated infections,” Esterman said.
Those who are more vulnerable may still be at risk from serious infections.
“For vulnerable people—that is, those who are elderly or have underlying health issues—they are at risk of severe illness,” Esterman said. “They should ensure that they are up to date with their booster shots against COVID-19 and start wearing an N95/P2 face mask when on public transport or shopping, etc. They should also have a plan in place with their family practice to make sure they have quick access to antivirals.”
If you do get a respiratory infection, he added, it is important to stay at home when possible so you avoid spreading it to others.
Is there a health problem that’s worrying you? Let us know via [email protected]. We can ask experts for advice, and your story could be featured in Newsweek.
Uncommon Knowledge
Newsweek is committed to challenging conventional wisdom and finding connections in the search for common ground.
Newsweek is committed to challenging conventional wisdom and finding connections in the search for common ground.

Rachel Carter is a health and wellness expert dedicated to helping readers lead healthier lives. With a background in nutrition, she offers evidence-based advice on fitness, nutrition, and mental well-being.